by Blake Christensen
edited by Glenn Baja
Is Lipitor the right drug for you? Are the side-effects something to be concerned about? Does it affect memory loss, cause erectile dysfunction, or increase the odds of getting prostate cancer? In fact, what is Lipitor? What is it meant to do? Is Lipitor a blessing or a curse?
The scope of this article is to take an objective look at these questions and come up with answers that will help you make an informed personal decision for yourself. Of course, be sure to consult your physician before making any final health decisions of your own.
Throughout my nursing career, there were 2 classes of drugs that seemed to be in every medication pass; blood pressure medications and cholesterol reducing drugs. Personally speaking, I’ve had experience with both. I have a family history of both hypertension (elevated blood pressure) and high cholesterol levels. I’ve been on several different blood pressure medications as well as 2 different cholesterol drugs. One of them was Lipitor, the most popular cholesterol-lowering medication on the market today.
Like anything with the aging body, we must look at the pros and cons of any actions we take to treat complications of the body. This is true of the drug Lipitor. The problem is high cholesterol. The solution may, or may not, be Lipitor. Yet, we cannot discuss Lipitor without a basic understanding of what cholesterol is, so let’s start there.
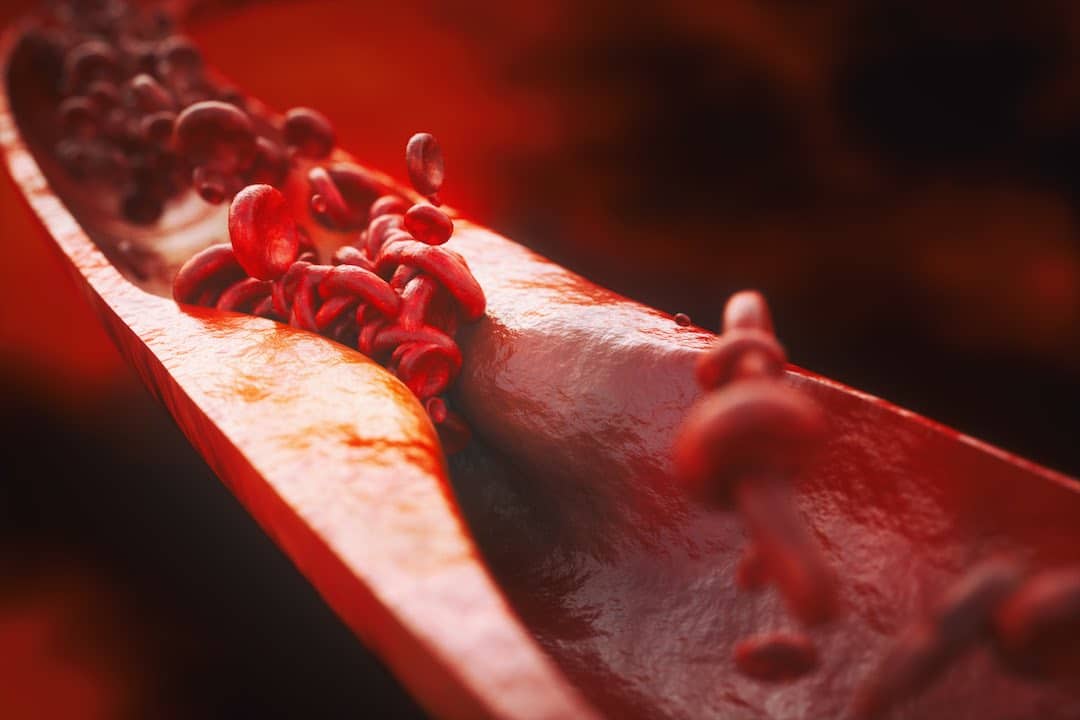
Blood Vessels filling up with Cholesterol
What Is Cholesterol?
Cholesterol is essentially a type of fat found in your blood. We need small amounts of blood cholesterol because our bodies use it to build the structure of cell membranes and partake in making hormones like estrogen, testosterone and adrenal hormones. Cholesterol also helps your metabolism work efficiently. For example, cholesterol is essential for your body to produce vitamin D.
Your liver makes 75% of the cholesterol in your bloodstream. The foods you eat make up the other 25%. The most common sources of foods that have cholesterol are meat, fish, eggs, butter, cheese, and milk. Problems arise when too much cholesterol exist in our bloodstream. When this happens, it can build up in deposits called plaque along the inside walls of arteries, causing them to narrow and constrict. In turn, this leads to blood flow restrictions which can lead to heart disease and stroke.
There are essentially two main types of cholesterol. One is called low-density lipoproteins (LDL) and the other, high-density lipoproteins (HDL). Low-density lipoproteins (LDL), the primary focus of this article, is sometimes called “bad” cholesterol. Elevated levels of this “bad” protein are what cause us problems.
LDL cholesterol is the type of cholesterol that builds up on the inside of the artery walls causing the formation of a hard, thick, substance called cholesterol plaque. This plaque thickening leads to a condition called atherosclerosis, which can lead to coronary heart disease and strokes.
__________
9 Interesting Facts About Cholesterol
-
- There is no minimum for dietary cholesterol. You don’t need to ingest foods to maintain cholesterol levels in your body.
- High cholesterol can be hereditary.
- Even children can have high cholesterol.
- Saturated fats (a type of fat considered to be less healthy in the diet than unsaturated fat) and trans fats (a type of unsaturated fat that has become widely produced industrially from vegetable fats for use in margarine, snack foods, packaged baked goods, and for frying fast food) matter more.
- Even modest weight loss can improve cholesterol levels.
- In women, cholesterol levels often rise after menopause.
- Small bumps on the skin (xanthomas) can be a sign of high cholesterol.
- Very low levels of total cholesterol may increase some health risks.
- Your doctor may not explain to you some of the above facts.
_______________
I must comment on fact number 9 in the above list. The traditional training of American physicians is comprehensive in nature. Their training revolves mainly in the diagnosis and treatment of diseases. Of interest is that nutrition classes are sorely missing in most medical school programs.
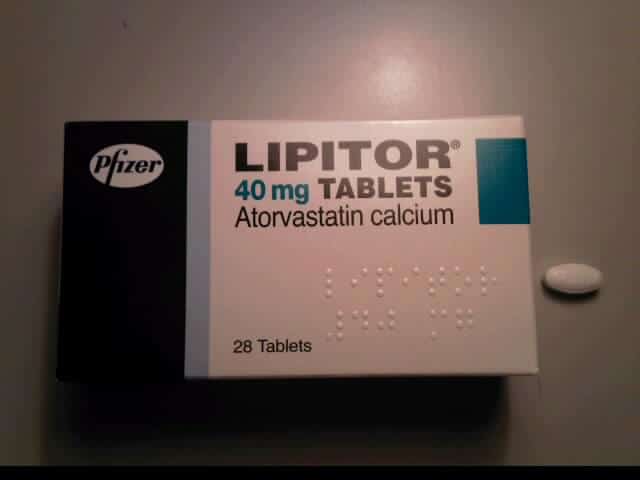
What Is Lipitor?
Lipitor is a brand name of a statin. Statins are any of a group of drugs that act to reduce levels of fats (cholesterol) in your blood. This includes triglycerides (the main component of natural fats and oils) and “bad” LDL cholesterol. They also increase levels of “good” HDL cholesterol. They are primarily used in the treatment of high blood cholesterol. However, statins don’t remove the plaque that’s already in your arteries or reduce blockages that already exist.
Doctors often prescribe Lipitor and other statins to treat dyslipidemia (elevated amounts of blood cholesterol, triglycerides, or both that contributes to the development of atherosclerosis) in the blood and to prevent cardiovascular disease (CVD) in those who are at high risk.
Best Selling Prescription Drug
Lipitor is the best-selling prescription drug in world history. It easily comes in at number one. It has been around longer and has 40% greater profit margin than its nearest competitor Humira. Approved in 1996, lifetime sales through 2016 is a staggering $148,744 million. In real numbers, that’s $148,744,000,000. Even with Lipitor’s patent ending in November 2011 (there is now several statins on the market, including generic Atorvastatin), Lipitor still holds a dominant position in the statin market.
Most MD’s are keenly aware of cardiac risk factors. When visiting your primary care physician, in almost all cases, they will order what is called a lipid panel test (a measurement of the fats in your blood).
In nature, the concept of cause and effect is alive and well. As the saying goes, you are what you eat. As a result, many of us in the United States pay a high price for eating excessive amounts of fatty foods. Fortunately for Pfizer, the giant drug company that makes Lipitor, we continue to love our cheeseburgers and French fries. The effect is increased cholesterol levels for us, and a fortune made by Pfizer Pharmaceuticals.
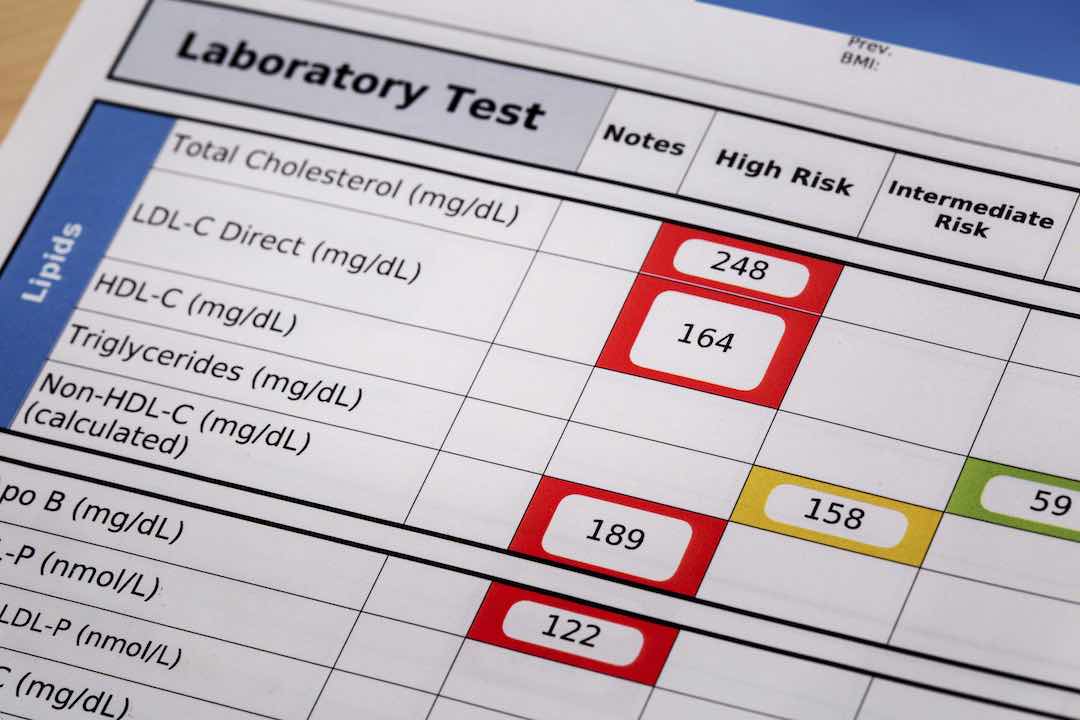
What Cholesterol Test Numbers Should I Know?
According to the latest data from Web MD, if you have a lipoprotein profile, it’s important to look at all the numbers from the cholesterol test, not just the total cholesterol number. That’s because LDL and HDL levels are two primary indicators of potential heart disease. Use the information below to interpret your results (with the help of your doctor, of course). This will help you get a better idea about your risk for heart disease.
Total blood cholesterol level:
- High risk: 240 mg/dl and above
- Borderline high risk: 200-239 mg/dl
- Desirable: Less than 200mg/dl
LDL cholesterol levels:
- High risk: 160 mg/dl and above
- Borderline high risk: 130-159 mg/dl
- Acceptable: 100-129
- Desirable: Less than 100mg/dl
HDL cholesterol levels:
- High risk: 40 mg/dl and below
- Borderline high risk: 41-59 mg/dl
- Desirable: 60mg/dl or higher
Standard Dosages
The recommended starting dose of LIPITOR is 10 or 20 mg once daily. Patients who require a large reduction in LDL may be started at 40 mg once daily. The acceptable dosage ranges of LIPITOR are 10 to 80 mg/day.
LIPITOR can be administered as a single dose at any time of the day, with or without food. The starting dose and maintenance doses of Lipitor should be individualized according to patient characteristics such as goal of therapy and response. After initiation and/or upon titration of Lipitor, lipid levels should be analyzed within 2 to 4 weeks and dosage adjusted accordingly.
More than 31 percent of all Americans have LDL levels that are too high. Almost 28 percent of Americans ages 40 to 59 use a cholesterol-lowering medication. People with high LDL levels have twice the risk of heart disease compared to people with healthier cholesterol levels, according to the Centers for Disease Control and Prevention (CDC).
Why Lipitor?
By Panthro at English Wikipedia, CC BY-SA 3.0, Link
What differentiates Lipitor from other statins is that it reduces more cholesterol at lower doses compared to the competition. The typical starting dose for Lipitor is 10 milligrams daily, and it can be prescribed at levels of up to 80 milligrams daily, whereas other statins are typically prescribed in amounts of 20 to 40 milligrams daily. When doctors first began prescribing statins, many were worried about long-term effects of high doses. While some of Lipitor’s early success is somewhat psychological, the effectiveness of lower doses makes Lipitor more attractive than other similar medications that require larger doses and potentially more side effects.
Lipitor And Statin Side-Effects
Many of the side effects of Lipitor do not normally need medical attention. Many may go away during treatment as your body adjusts to the medicine. According to WebMD, the following are some of the side effects you may experience from Lipitor usage:
Common Side Effects
-
- Joint Pain (the most common side effect)
- Diarrhea
- Indigestion
- Pain or tenderness around the eyes and cheekbones
- Urinary Tract Infection
- Throat Irritation
Infrequent Side Effects
-
- Muscle pain/muscle spasm (the most common infrequent side effect)
- Rash
- Muscle or bone pain
- Dizziness
- Chronic trouble sleeping
- Vomiting, or feeling like you are going to vomit
RARE Side Effects (Partial List)
The most common rare effects are:
-
-
- Liver failure
- Hepatitis
- Pancreatitis
- Giant hives
- Lung tissue problems
-
The less common rare side effects are:
-
-
- Blurred vision
- Confusion
- Depression
- Nightmares
- Joint stiffness
-
Note: In the analysis of 135 previous studies, which included nearly 250,000 people combined, researchers found that the drugs simvastatin (Zocor) and pravastatin (Pravachol) had the fewest side effects of the statins. They also found that lower doses produced fewer side effects in general.
According to the Mayo Clinic, not everyone who takes a statin will have side effects, but some people may be at a greater risk than are others. These factors include:
- Taking multiple medications to lower your cholesterol
- Being female
- Having a smaller body frame
- Being age 65 or older
- Having kidney or liver disease
- Drinking too much alcohol
Lipitor and Memory Loss
In a 2013 review, independent and unsponsored researchers from Johns Hopkins Medicine looked at 41 different studies on various statins to see if there was a link between taking the medication and memory loss. The studies looked at 23,000 men and women who showed no prior history of memory problems in the prior 25 years.
The dozens of studies showed that using statins to control cholesterol levels posed no threat to short-term memory. Studies suggested that prolonged use of statins for over one year may even help protect against dementia, reducing its risk by up to 29 percent. According to senior author Seth Martin, M.D.:
“Because of their effect on arteries to reduce or stabilize plaque, and prevent strokes, it makes sense that statins could be protective in the brain against dementia.”
These results should offer more clarity and reassurance to end users and the doctors who prescribe the statin medications that are concerned about memory loss.
However, it is important to consider that taking multiple medicines could theoretically interact with each other and cause cognitive problems.
Lipitor Side-Effects in Men
There has been plenty of discussions whether statin use (including Lipitor) has any side-effects in men. The predominant concerns are whether these drugs have any impact on erectile dysfunction problems or expose men to a higher risk of prostate cancer. As you will see, in many of these cases the “jury” is still out.
Erectile Dysfunction
While ED isn’t a widely reported side-effect of statins, researchers have explored the possibility in many different studies. One 2014 study in the Asian Journal of Andrology found that statins may, in fact, reduce testosterone levels. Testosterone is the primary male sex hormone, and it’s necessary for an erection to be achieved. Yet, the same study found that over time, ED improved among men who were taking statins for high cholesterol.
“Therefore, our results indicate that statins were associated with a significant improvement in erectile function.”
~ Asian Journal of Andrology
A 2017 review in the American Journal of Medicine found that statins didn’t increase men’s risk of sexual dysfunction, although researchers agreed that more study is needed.
“Among men with established cardiovascular disease or cardiovascular disease risk factors, statin use does not seem to be associated with a new onset of erectile dysfunction.”
~American Journal of Medicine
The Mayo Clinic states that clogged arteries can cause ED. This shouldn’t come as a surprise considering that an erection is dependent upon blood flow to the penis. It may not be the statin medication itself causing problems, but rather the clogged arteries themselves may be the cause. Clogged arteries affect not only the blood vessels supplying the heart, but also blood vessels throughout the entire body.
Atherosclerosis affects different people in different places, but it often affects the penis first. In fact, a 2011 report found that ED is sometimes a warning sign that a person could have a heart attack or stroke within the next 3 to 5 years.
ED may be a blessing in disguise if it alerts you and your doctor that you have atherosclerosis, especially if it helps prevent a heart attack or stroke in the future.
Risk of Prostate Cancer
According to a number of studies published in the Cancer Therapy Advisory, the use of statins is associated with a decreased risk in prostate cancer mortality. Similarly, according to a study published in the Journal of Clinical Oncology, patients who take statins after prostate cancer diagnosis may have a reduced risk of mortality. However, they go on to say that:
“… the effect of statins on prostate cancer is complex, with laboratory evidence indicating that statins can have both pro- and anti-neoplastic effects, and previous studies yielding mixed results.”
But there is a flip side. Statins, cheered for their ability to lower cholesterol levels, may have a dark side that includes evidence that they may be associated with an increased risk of prostate cancer. Results of this study, published in the December 2011 issue of Prostate, contradicts previous research that has explored any association between statin use and prostate cancer risk.
This new study unquestionably raises more questions than it answers. Unfortunately, with so many contradicting studies out there, the quest for whether statins are beneficial or hazardous to prostate health, or have a role in prostate cancer, is still uncertain.
It is important for men to do their own research and consult with their healthcare providers before making any decisions before taking Lipitor or any other statin drugs.
Lastly
During my 28 years in nursing, I have a story to share regarding medication side effects. On numerous occasions, I have walked into a patient’s room to see them deeply concentrating and reading a Physicians’ Desk Reference drug book. It does not matter what drug book they were reviewing. In the back of my mind, I’m thinking, “here we go!” I am referring to the medication side-effect battle. Is the medication worth taking?
Fortunately, as a nurse, I could always refer them to a pharmacist or their attending physician. My opinion has remained constant. In most cases, the benefits of taking Lipitor are worth the risk.
Bottomline
In this article, we have reviewed the problem: high cholesterol levels. We have investigated the extremely successful drug Lipitor. And along the way learned some fun facts regarding cholesterol. So, what is the bottom line, the takeaway from this information?
-
- All patients, regardless of the setting, have the right to take part in their care. This includes the medications they take. This article is intended to educate you. It is intended to assist you in making an informed decision.
- There are many good medications on the market and when taking medications always consider the pros and cons regarding usage. In my professional opinion, the pros of taking Lipitor far outweigh the cons; however, in my personal situation, one con outweighed the pros.
- There are always alternatives to taking medications, such as lifestyle changes (diet, exercise).
- It is always best to be well informed regarding your medical care. I often refer to websites such as Web MD and the Mayo Clinic.
In my situation, I took Lipitor for several weeks. One day I woke up and I felt like I had been hit by a train. The muscle aches were incredible. A week later, while continuing Lipitor, my aches were not improving. Muscle aches are listed as a minor side effect of Lipitor. I could only wonder about the more serious side effects. I double checked the medical literature, made an informed decision, and stopped taking Lipitor. Instead, I made some simple dietary changes. A year later my cholesterol levels were fine.
Educate yourself about your options and research all you can on the drugs you’re thinking of taking. Today, we ultimately need to personally partake in choosing our own health paths. It is up to us to choose the one that best suits and promotes our own health care needs.
About the Author
Blake Christensen is a freelance writer who currently resides in the Philippines.
He is a Vietnam Era Veteran (US Army Medical Corpsman) and describes himself as “Your classic Baby Boomer hippie gone conservative.”
He graduated from The University of Texas Health Sciences Center in Houston with a BSN. Areas of clinical nursing: Critical care, emergency, prison nursing, psychiatry, geriatric medicine. Advanced studies at The University of Southern California Davis School of Gerontology.
He is an avid golfer and scuba diver. But his true love is gerontology and how we can all age well.
I’m a self-professed madman, adventurer, photographer, certified High-Performance Coach, martial artist, and licensed physical trainer specializing in senior fitness. My passion is to continue growing and developing into my own unique, gifted, and joyful authenticity, while committing myself towards doing my own special part to help change the world. My mission is to help others find their own direction and purpose in life, by means of mentoring, teaching, and empowering.